Why physiotherapy matters after back surgery for faster recovery
- 11 hours ago
- 9 min read

TL;DR:
Physiotherapy accelerates healing, restores muscle strength, and improves spinal stability after back surgery.
Early, supervised rehabilitation enhances pain relief, reduces disability, and lowers reliance on pain medication.
Different surgical procedures impact physiotherapy outcomes, with non-fusion surgeries showing more consistent benefits.
After back surgery, the instinct is to rest and let your body heal on its own. But rest alone will not restore the muscle strength, spinal stability, or mobility you need to return to normal life. Research confirms that physiotherapy significantly reduces pain, disability, and recovery time following lumbar disc surgery, with evidence drawn from 55 randomised controlled trials involving over 4,300 patients. If you are recovering from back surgery in Bedfordshire or Buckinghamshire, this guide explains exactly how physiotherapy accelerates your rehabilitation, what to expect at each stage, and how to apply this knowledge safely.
Table of Contents
Key Takeaways
Point | Details |
Early physiotherapy boosts recovery | Starting physiotherapy soon after surgery restores mobility and reduces pain faster. |
Supervision is vital | Expert-led rehabilitation is safer and more effective than unsupervised home exercise. |
Pain and medication decreases | Physiotherapy lowers pain and reduces opioid use post-back surgery. |
Safety first | Avoid heavy lifting and running in the first months to prevent complications during recovery. |
Why physiotherapy is critical after back surgery
Many patients leave hospital with a list of restrictions and an expectation that time will do the healing. In reality, the muscles surrounding your spine weaken rapidly after surgery, and passive rest does very little to restore them. Without targeted intervention, stiffness, weakness, and compensatory movement patterns can become long-term problems that outlast the original injury.
Physiotherapy works by systematically reactivating and rebuilding the structures that support your spine. Targeted exercises such as transversus abdominis activation, structured walking progression, and postural training strengthen core and back muscles, improve flexibility, and restore function. These are not generic gym exercises. They are precision movements designed to protect surgical repair while loading the tissue in ways that encourage healthy healing.
The evidence is robust. A large-scale review confirms that physiotherapy reduces pain, disability, and improves quality of life following lumbar disc surgery, with 55 randomised trials confirming the efficacy of back muscle strengthening and flexibility exercises across thousands of patients.
Key reasons physiotherapy is essential after back surgery:
Muscle atrophy begins within days of surgery without active rehabilitation
Scar tissue can restrict movement unless managed with appropriate exercise and manual therapy
Pain sensitisation reduces without graded, supervised activity
Confidence and movement fear improve significantly with structured, professional support
Posture and gait normalise more quickly with expert guidance
“Physiotherapy is not just about recovery. It is about reclaiming the physical capacity that surgery itself cannot restore.” The operation addresses the structural problem. Rehabilitation rebuilds the function around it.
Understanding this distinction is important. Surgery removes the source of nerve compression or instability. Evidence-based physiotherapy then addresses the functional consequences: weakness, altered movement, and chronic pain patterns that persist even after a technically successful operation.
Once the value of physiotherapy is established, we can explore the practical stages of rehabilitation.
Stages of physiotherapy rehabilitation
Physiotherapy after back surgery is not a single programme. It is a progression of carefully sequenced phases, each building on the last. Understanding the structure helps you set realistic expectations and recognise when you are ready to advance.
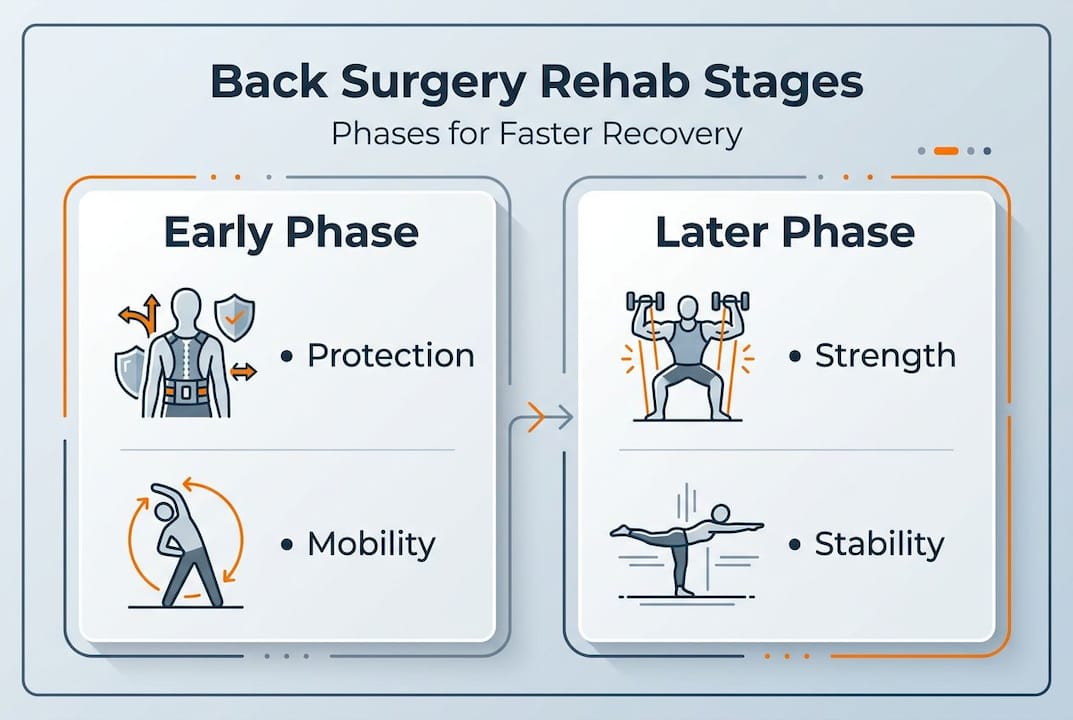
Phase 1: Protection and mobility (weeks 1 to 2). The priority immediately after surgery is protecting the surgical site whilst preventing stiffness. Exercises begin straight away, starting with pelvic floor tightening, gentle knee flexion and extension, and ankle pumps to maintain circulation. Walking is introduced gradually and increased day by day.
Phase 2: Strengthening (weeks 3 to 6). As your surgical site stabilises, the focus shifts to rebuilding core stability and spinal support. Exercises become more demanding, introducing bridging, supported squats, and controlled abdominal engagement. Swimming can typically begin around four weeks, offering low-impact resistance that supports muscle recovery.
Phase 3: Functional return (beyond six weeks). The final phase bridges the gap between rehabilitation and real life. Step by step physiotherapy recovery at this stage involves sport-specific or work-specific movements, progressive loading, and a structured return to full activity. Research confirms that combining exercise, education, and manual therapy produces the best outcomes across all three phases.
Phase | Timeline | Focus | Example exercises |
Protection and mobility | Weeks 1 to 2 | Prevent stiffness, protect healing | Pelvic floor, knee flex, walking |
Strengthening | Weeks 3 to 6 | Core stability, muscle rebuilding | Bridging, swimming, abdominal work |
Functional return | Beyond 6 weeks | Return to daily life and activity | Progressive loading, sport-specific drills |
Pro Tip: Never skip Phase 1 to accelerate progress. The protection phase creates the foundation every subsequent stage depends on. Rushing it increases the risk of setback significantly.
Your physiotherapist will adapt the programme based on your surgical type, fitness levels, and how your body responds. Home exercises for back recovery between supervised sessions are important, but they work best when designed and monitored by a professional.
Understanding each stage helps set expectations for your recovery journey.
Comparing physiotherapy outcomes: Fusion vs non-fusion procedures
Not all back surgeries are the same, and the research shows that the type of operation you have had affects how strongly physiotherapy influences your recovery. This is an important distinction that many general guides overlook entirely.
For patients who have undergone spinal fusion, the evidence is more mixed. A review of 31 studies involving 4,335 patients found that physiotherapy produced 43% pain benefit in lumbar fusion cases, meaning pain improvement was documented in just 3 of 7 relevant studies. This does not mean physiotherapy is ineffective after fusion. It means the evidence is less consistent, and expectations should be managed accordingly.
For non-instrumented procedures such as discectomy, the picture is considerably clearer. The same research found a 63% pain relief rate in non-fusion patients, with more consistent evidence for reductions in both pain and disability. The structural simplicity of these procedures appears to allow physiotherapy to produce more predictable results.
Surgery type | Pain benefit evidence | Disability improvement | Evidence consistency |
Lumbar fusion | 43% (3 of 7 studies) | Moderate | Mixed |
Non-fusion (e.g. discectomy) | 63% | Strong | Consistent |
Practical takeaways for patients:
If you have had a fusion procedure, physiotherapy remains important, but recovery timelines may be longer and less linear
If you have had a discectomy or similar non-fusion surgery, evidence for physiotherapy effectiveness strongly supports early and consistent engagement
In both cases, supervised physiotherapy outperforms unsupervised exercise
Discuss your specific procedure with your physiotherapist so the programme reflects your actual surgery
These beginner physiotherapy tips are a useful starting point, but the most effective approach is one tailored to your individual surgical history and current physical condition.
With outcome differences in mind, it is important to address how physiotherapy influences pain management and medication use.
Reducing pain, disability, and opioid use
One of the most compelling arguments for physiotherapy after back surgery is its documented ability to reduce dependence on pain medication. This matters enormously for long-term health and quality of life.
Studies show that patients who engage in post-operative physiotherapy have a significantly lower risk of needing opioid prescriptions. Research on cervical fusion patients found that physiotherapy was associated with a relative risk of 0.739 for oral opioid use, meaning a nearly 27% reduction in opioid prescription risk compared to those without physiotherapy. Translated into everyday terms: engaging with your physiotherapist actively reduces the likelihood that you will need strong painkillers to manage your recovery.
Beyond opioid reduction, the impact on disability is equally significant. A meta-analysis found that complex rehabilitation combining exercise with cognitive behavioural approaches reduces disability with an effect size of 0.85 in the short term, effects that are maintained long-term with consistent rehabilitation engagement.
Key benefits for patients choosing supervised physiotherapy:
Reduced pain through graded exercise and manual therapy techniques
Lower medication reliance and fewer prescription-related side effects
Decreased disability through functional movement restoration
Improved quality of life as independence is regained progressively
Better psychological outcomes as fear of movement reduces with structured guidance
“Pain after surgery is not always a signal to stop. With supervised physiotherapy, patients learn to distinguish between productive discomfort and genuine warning signs, which is a skill that transforms recovery.”
Pro Tip: If you are finding it difficult to manage pain without medication, discuss this directly with your physiotherapist. They can modify your programme and use methods for pain reduction including manual therapy, soft tissue work, and acupuncture to support more comfortable progression.
Having explored pain management, the next step is safe, practical application for Bedfordshire and Buckinghamshire patients.
Safety, supervision, and practical strategies for Bedfordshire and Buckinghamshire
Starting physiotherapy safely after back surgery requires knowing what to do, what to avoid, and when professional guidance is non-negotiable. Research is clear that early supervised exercise, beginning as soon as day one post-surgery, produces better outcomes than delayed or unsupervised rehabilitation.
However, early does not mean aggressive. There are firm boundaries to respect. Evidence recommends avoiding neural mobilisation, heavy lifting for at least six weeks, and running for up to six months following lumbar surgery. Monitoring for complications such as infection, increased neurological symptoms, or falls is also essential during the early recovery window.
Activity | Restriction period | Reason |
Neural mobilisation | Avoid early post-op | Risk of nerve irritation |
Heavy lifting | Minimum 6 weeks | Surgical site protection |
Running | Up to 6 months | Spinal load management |
Swimming | From approximately week 4 | Supported low-impact exercise |
Common mistakes patients in our region make during recovery:
Progressing too quickly based on how good they feel on a given day
Skipping supervised sessions in favour of independent home exercise
Returning to driving or prolonged sitting before clearance is given
Ignoring signs of infection or unusual pain at the surgical site
Pro Tip: Keep a simple daily log of pain levels, activity, and any unusual symptoms during the first eight weeks. This gives your physiotherapist the information they need to adapt your programme accurately and helps you notice patterns that could indicate a complication.
For patients across Bedfordshire and Buckinghamshire, accessing essential tips for recovery and professionally guided top home exercises between sessions helps maintain consistency without overloading the recovering spine.
A fresh perspective: What most guides overlook about post-surgical physiotherapy
Conventional post-surgical guidance often errs heavily on the side of caution. Patients are told to rest, avoid bending, and wait. Whilst these instructions have their place, they can become obstacles when followed too rigidly.
The reality is that there is no strong evidence supporting extended activity restrictions beyond the basics. Supervised physiotherapy consistently outperforms home exercise alone, yet many patients receive a sheet of generic exercises and little else after discharge.
For fusion surgery specifically, the debate continues. Timing, cost-effectiveness, and whether rehab accelerates healing or risks overload are still being researched. What we know from real-world clinical experience is that patients who engage early, under professional supervision, tend to do better regardless of the procedure type.
The uncomfortable truth is that fear of movement often does more damage than movement itself. Structured, supervised physiotherapy produces measurable results precisely because it teaches patients to move again with confidence. That shift in mindset, supported by a skilled physiotherapist, is frequently what separates a smooth recovery from a prolonged struggle.
Connect with expert physiotherapy support
If you are recovering from back surgery in Bedfordshire or Buckinghamshire, having the right team around you makes a genuine difference to your outcome. Supervised physiotherapy is not a luxury. It is the evidence-based standard for optimal recovery.

At The Parks Therapy Centre, our physiotherapists have supported patients through post-surgical rehabilitation since 1986. We understand the nuances of different surgical procedures, the importance of staged progression, and how to adapt programmes for each individual. Whether you are in the early protection phase or working towards full functional return, we offer expert physiotherapy in Bedfordshire and Buckinghamshire with online booking available. Take the next step towards a stronger, more confident recovery today.
Frequently asked questions
How soon should I begin physiotherapy after back surgery?
Patients often start gentle supervised exercises from day one after surgery, with home routines typically introduced between two and six weeks post-operation depending on the procedure and individual recovery.
Are there risks or activities I should avoid after back surgery?
You should avoid neural mobilisation, heavy lifting for at least six weeks, and running for up to six months, whilst monitoring for complications such as infection or falls throughout early recovery.
Does physiotherapy reduce pain medication use after surgery?
Yes. Research shows physiotherapy significantly lowers the risk of opioid prescriptions after back surgery, with a relative risk reduction of approximately 27% compared to patients without post-operative physiotherapy.
What benefits can I expect from supervised physiotherapy?
Supervised physiotherapy delivers better pain reduction, improved mobility, and measurably lower disability than home exercise alone, as confirmed by 55 randomised trials involving thousands of post-surgical patients.
Recommended
