Vestibular rehabilitation: restore balance with expert therapy
- 1 day ago
- 8 min read

TL;DR:
Vestibular rehabilitation therapy is exercise-based treatment targeting inner ear balance issues.
Customized programs and professional supervision significantly improve recovery outcomes.
Most patients see improvement within 4 to 12 weeks, with early intervention being most effective.
Dizziness is one of those symptoms people tend to dismiss, assuming it will pass on its own. For many, it does not. Persistent dizziness, unsteadiness, and balance loss can quietly erode confidence, restrict movement, and raise the risk of serious falls. Vestibular rehabilitation therapy (VRT) is a clinically proven approach that targets the root causes of these problems rather than masking them. This article explains what VRT involves, who it suits, what a typical programme looks like, and what results you can realistically expect, so you can make an informed decision about your next step.
Table of Contents
Key Takeaways
Point | Details |
Supervised rehab works best | Working with a professional ensures faster, safer recovery from dizziness and balance loss. |
Customisation matters | Tailoring therapy to your diagnosis and symptoms is critical for lasting improvement. |
Early action accelerates progress | Starting vestibular rehab soon after symptoms appear leads to better outcomes and mobility. |
Temporary symptoms are normal | Initial increases in dizziness are typical but fade as therapy progresses—serious risks are rare. |
New technologies emerging | Virtual reality and augmented feedback may further enhance rehab results as adjuncts in future programmes. |
What is vestibular rehabilitation physical therapy
Vestibular rehabilitation physical therapy is a specialist form of exercise-based treatment designed to address dizziness, vertigo, and imbalance caused by problems in the vestibular system. The vestibular system sits within the inner ear and works with the brain and eyes to control balance and spatial orientation. When it malfunctions, the signals your body relies on to stay upright become unreliable.
Conditions commonly treated through vestibular rehab include:
Benign paroxysmal positional vertigo (BPPV): Brief, intense spinning triggered by head movement
Vestibular neuritis: Inflammation of the vestibular nerve, often following a viral illness
Unilateral hypofunction: Reduced function on one side of the vestibular system
Bilateral hypofunction: Loss of function on both sides, often from medication toxicity or ageing
Labyrinthitis: Inflammation affecting both hearing and balance
The goal of VRT is threefold: restore postural stability, improve gaze control (the ability to keep vision steady during movement), and reduce the risk of falls. A physiotherapist designs a personalised programme using specific exercises that encourage the brain to adapt and compensate for vestibular deficits. This process is called central compensation.
“Vestibular rehabilitation is a safe, effective intervention that reduces dizziness, improves stability, lowers fall risk in people with peripheral vestibular disorders.”
What sets VRT apart from medication is its lasting effect. Drugs can suppress symptoms temporarily, but they do not retrain the brain. For peripheral vestibular loss, where the problem originates in the inner ear rather than the brain itself, exercise-based therapy consistently outperforms medication alone over the long term. Patients who commit to their programme often describe a gradual but meaningful return to activities they had given up, from driving and cooking to walking confidently without holding on to walls.
Who should consider vestibular rehab: eligibility and contraindications
Not everyone with dizziness will benefit from VRT, and understanding eligibility is essential before starting. The therapy is most effective for peripheral vestibular disorders, meaning conditions originating in the inner ear or vestibular nerve rather than the central nervous system.
Here is a straightforward guide to suitability:
Peripheral vestibular disorders such as BPPV, vestibular neuritis, and unilateral or bilateral hypofunction are the primary indications
Chronic dizziness that has persisted for more than three months and has not resolved with rest
Post-concussion balance problems where vestibular involvement is confirmed
Age-related balance decline where supervised exercise can reduce fall risk
Post-surgical vestibular changes following acoustic neuroma removal or inner ear procedures
Suitable for VRT | Caution or contraindicated |
Peripheral vestibular disorders | Active Meniere’s disease attacks |
Chronic unilateral/bilateral hypofunction | Severe cognitive impairment |
BPPV (with repositioning manoeuvres) | Uncompensated central vestibular disorders |
Post-concussion vestibular symptoms | Acute cardiovascular instability |
Age-related balance decline | Recent onset without medical clearance |
APTA guidelines recommend supervised VRT for various hypofunctions, while clearly outlining edge cases and contraindications that require clinical judgement. Central vestibular disorders, such as those caused by stroke, tumours, or multiple sclerosis, require a different treatment pathway entirely.
For older adults or those with multiple health conditions, a customised and closely supervised plan is especially important. Falls during unsupervised exercise are a real risk when balance is already compromised. Reviewing physiotherapy recovery tips before starting can help you prepare practically and mentally.

Pro Tip: Always obtain a confirmed diagnosis before beginning VRT. Starting exercises without knowing whether your dizziness is peripheral or central can delay the correct treatment and, in rare cases, cause harm.
What to expect: typical vestibular rehab programme and timeline
A vestibular rehabilitation programme is not a one-size-fits-all set of exercises. It is a structured, progressive plan built around your specific deficits and goals. That said, most programmes share a common framework.
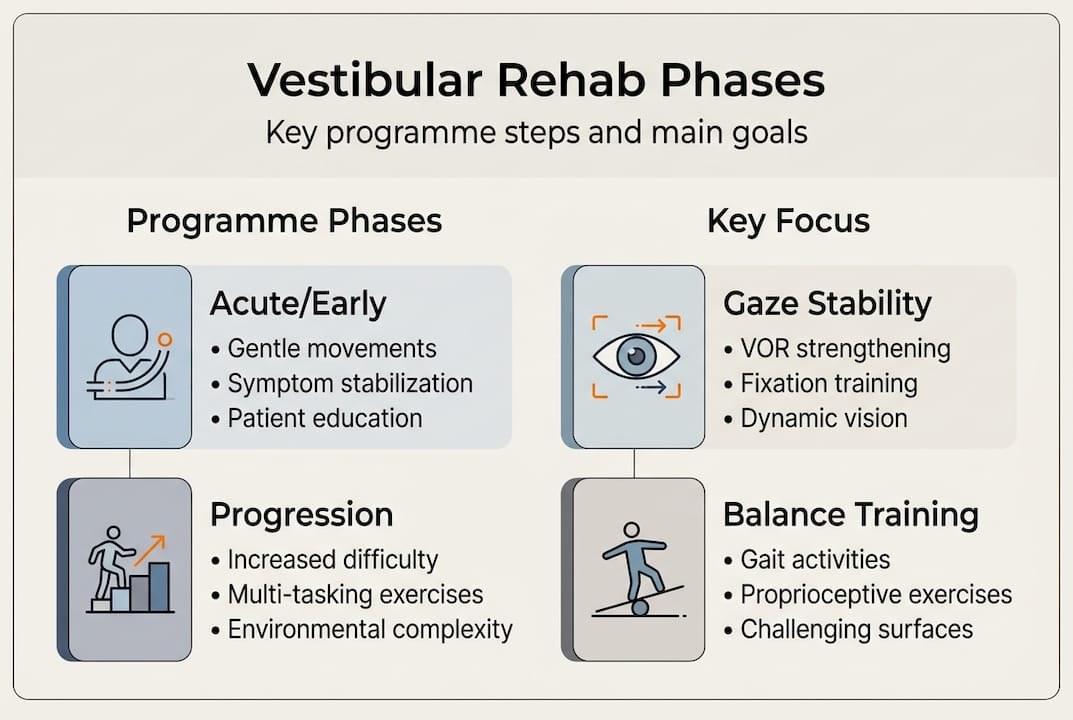
Core components of a VRT programme:
Gaze stabilisation exercises: Training the eyes to hold focus while the head moves, reducing visual blurring and dizziness
Balance training: Standing and moving tasks that challenge stability on different surfaces
Walking exercises: Gait retraining to improve confidence and coordination
Canalith repositioning manoeuvres: Specific head movements (such as the Epley manoeuvre) used for BPPV
Habituation exercises: Repeated exposure to movements that provoke dizziness, gradually reducing sensitivity
Programme phase | Typical duration | Key focus |
Acute/early | Weeks 1 to 2 | Assessment, gentle gaze and balance exercises |
Mid-programme | Weeks 3 to 6 | Progressive balance, walking, habituation |
Late/consolidation | Weeks 7 to 12 | Functional tasks, independence, fall prevention |
Gaze exercises 3 to 5 times daily, balance training for 20 or more minutes each day, and an overall programme length of 4 to 12 weeks are the benchmarks supported by clinical guidelines. Chronic cases or those with bilateral loss may require longer.
One thing that surprises many patients: symptoms can feel temporarily worse in the first week or two. This is normal. Temporary dizziness increases are common at the start of VRT, and no serious adverse effects have been reported in clinical studies. Think of it like the muscle soreness after starting a new fitness routine. It signals that adaptation is happening.
Pro Tip: Keep a simple symptom diary during your programme. Tracking dizziness levels daily helps your physiotherapist adjust the plan and shows you how far you have come, which is genuinely motivating during harder weeks.
Integrating home physiotherapy exercises between clinic sessions accelerates progress, and for those who enjoy structured movement, Pilates in rehab can complement vestibular training by building core stability and body awareness.
Customisation, outcomes, and emerging trends in vestibular rehab
The evidence for VRT is strong, but the quality of outcomes depends heavily on how well the programme is tailored to the individual. Generic exercise sheets handed out without assessment rarely produce the same results as a properly customised plan.
What drives better outcomes:
Early intervention, ideally within the first few weeks of symptom onset
Programmes matched to the specific type and severity of vestibular loss
Regular reassessment and progression by a qualified physiotherapist
Addressing anxiety and fear of movement, which often develop alongside balance problems
Combining VRT with appropriate medication where indicated
For vestibular neuritis specifically, combining medication with rehab improves outcomes compared to either approach alone, with virtual reality and augmented feedback technologies emerging as promising adjuncts. These tools create immersive environments that challenge the vestibular system in controlled, repeatable ways, something that is difficult to replicate in a standard clinic setting.
A Cochrane review of VRT confirmed that customised vestibular rehabilitation shows clear superiority over generic or no treatment for acute unilateral peripheral vestibular disorders, with meaningful improvements in dizziness, postural stability, and quality of life.
Key outcomes patients report after completing VRT:
Significant reduction in dizziness frequency and intensity
Improved confidence walking on uneven ground or in busy environments
Lower fall rates and reduced fear of falling
Return to work, driving, and social activities
Choosing the right approach matters. Understanding physiotherapy techniques available to you helps you ask better questions and engage more actively in your own recovery. For those who want to stay well long term, injury prevention strategies provide a practical framework for maintaining the gains made through rehabilitation.
Why customisation and supervision are key for lasting results
Having reviewed the emerging evidence and worked alongside patients navigating vestibular disorders, one pattern is unmistakable: the people who recover fastest are not those who work hardest in isolation. They are those who receive the right exercises, at the right intensity, with regular expert review.
Generic vestibular exercise programmes downloaded from the internet are not without value, but they cannot account for your specific deficits, your comorbidities, or the way your symptoms change week by week. Supervised, customised programmes consistently show better adherence and faster recovery, particularly in chronic and bilateral cases where the stakes are higher.
There is also the psychological dimension. Balance disorders generate anxiety. Anxiety makes people avoid movement. Avoidance slows recovery. A skilled physiotherapist does not just prescribe exercises; they build your confidence, explain what is happening in your body, and keep you progressing when it feels uncomfortable. That relationship is part of the treatment. Seeking specialist vestibular rehab early, rather than waiting to see if symptoms resolve, is one of the most effective decisions you can make.
Get expert help for your vestibular rehab journey
If persistent dizziness or balance problems are affecting your daily life, professional support can make a meaningful difference to how quickly and fully you recover.

At Parks Therapy Centre, our experienced physiotherapists offer tailored vestibular rehabilitation programmes designed around your specific diagnosis, lifestyle, and goals. We provide safe, supervised treatment across multiple locations in Bedfordshire and Buckinghamshire, with online booking available for your convenience. Whether you are newly diagnosed or have been struggling with balance issues for months, our team is ready to help. Visit Parks Therapy Centre to book your initial assessment and take the first step towards restored confidence and mobility.
Frequently asked questions
How long does vestibular rehabilitation take to show results?
Most people notice meaningful improvement within 4 to 12 weeks, though chronic or complex cases may require a longer programme before significant gains are felt.
Will vestibular rehab make my symptoms worse?
A temporary increase in dizziness is common in the early stages, but no serious adverse effects have been reported, and most patients see steady improvement as the programme progresses.
Can home exercises replace supervised vestibular rehab?
Home exercises are a valuable part of recovery, but supervised programmes ensure exercises are correctly matched to your deficits and safely progressed, particularly in chronic or complex cases.
Is vestibular rehabilitation suitable for central balance disorders?
Clinical guidelines focus primarily on peripheral vestibular disorders; central causes of dizziness such as stroke or tumours typically require different specialist treatment pathways.
Recommended
