Why physiotherapy is essential for musculoskeletal disorders
- Mar 23
- 8 min read

Many adults with musculoskeletal disorders mistakenly believe rest alone will resolve their condition. This common misconception often leads to prolonged discomfort and delayed recovery. Physiotherapy offers targeted approaches that promote actual healing and restore function rather than simply masking symptoms. Whether you’re dealing with chronic pain, sports injuries, or post-operative rehabilitation in Bedfordshire and Buckinghamshire, understanding how physiotherapy addresses the root causes of your condition can transform your recovery journey. This guide explains why physiotherapy is crucial for effective musculoskeletal disorder management and how to access expert care locally.
Table of Contents
Understanding musculoskeletal disorders and physiotherapy’s role
How physiotherapy helps chronic pain, sports injuries, and post-operative recovery
Accessing physiotherapy for musculoskeletal disorders in Bedfordshire and Buckinghamshire
Current research and future directions in physiotherapy for musculoskeletal disorders
Key Takeaways
Point | Details |
Root causes focus | Physiotherapy targets root causes rather than simply masking symptoms to promote real recovery. |
Education and exercise | Pain neuroscience education combined with active exercises reduces chronic pain and improves function. |
Tailored rehabilitation plans | Individualised plans for sports injuries and post operative recovery optimise outcomes. |
NHS access routes | In Beds and Bucks, NHS pathways provide structured access to physiotherapy services. |
Understanding musculoskeletal disorders and physiotherapy’s role
Musculoskeletal disorders affect the bones, muscles, ligaments, tendons, and nerves that support your body’s movement and structure. These conditions range from acute sports injuries to chronic degenerative diseases, each presenting unique challenges to daily function. Common symptoms include persistent pain, stiffness, reduced range of motion, and weakness that interfere with work, leisure activities, and basic self-care tasks.
Physiotherapy addresses these conditions through physical methods that restore movement and reduce pain without relying solely on medication. Unlike passive treatments that provide temporary relief, exercise-based functional restoration combined with pain neuroscience education empowers you to take an active role in your recovery. This approach recognises that your nervous system’s response to pain often matters more than the structural damage itself.
Effective physiotherapy strategies prioritise how your body processes pain signals rather than focusing exclusively on mechanical alignment. When you understand the science behind your symptoms, you’re better equipped to engage with treatment and maintain progress. This educational component transforms physiotherapy from something done to you into a collaborative process you control.
Key principles that guide modern physiotherapy for musculoskeletal disorders include:
Progressive loading that gradually rebuilds tissue tolerance and strength
Movement pattern retraining to reduce compensatory habits that perpetuate pain
Pain education that reframes your understanding of discomfort as a protective mechanism
Functional goal setting that aligns treatment with your specific life demands
Self-management strategies that extend benefits beyond clinic sessions
For a comprehensive understanding of the treatment process, explore our step by step physiotherapy guide that walks you through each recovery phase.
Pro Tip: Keep a symptom diary tracking pain levels, activities, and sleep quality to help your physiotherapist identify patterns and adjust your treatment plan more precisely.
How physiotherapy helps chronic pain, sports injuries, and post-operative recovery
Chronic pain management through physiotherapy emphasises restoring function via exercise and education rather than passive treatments that provide only temporary relief. Research shows that manual therapy works through neurophysiological mechanisms rather than simply correcting structural problems. This understanding shifts treatment focus from fixing perceived tissue damage to modulating how your nervous system processes pain signals.
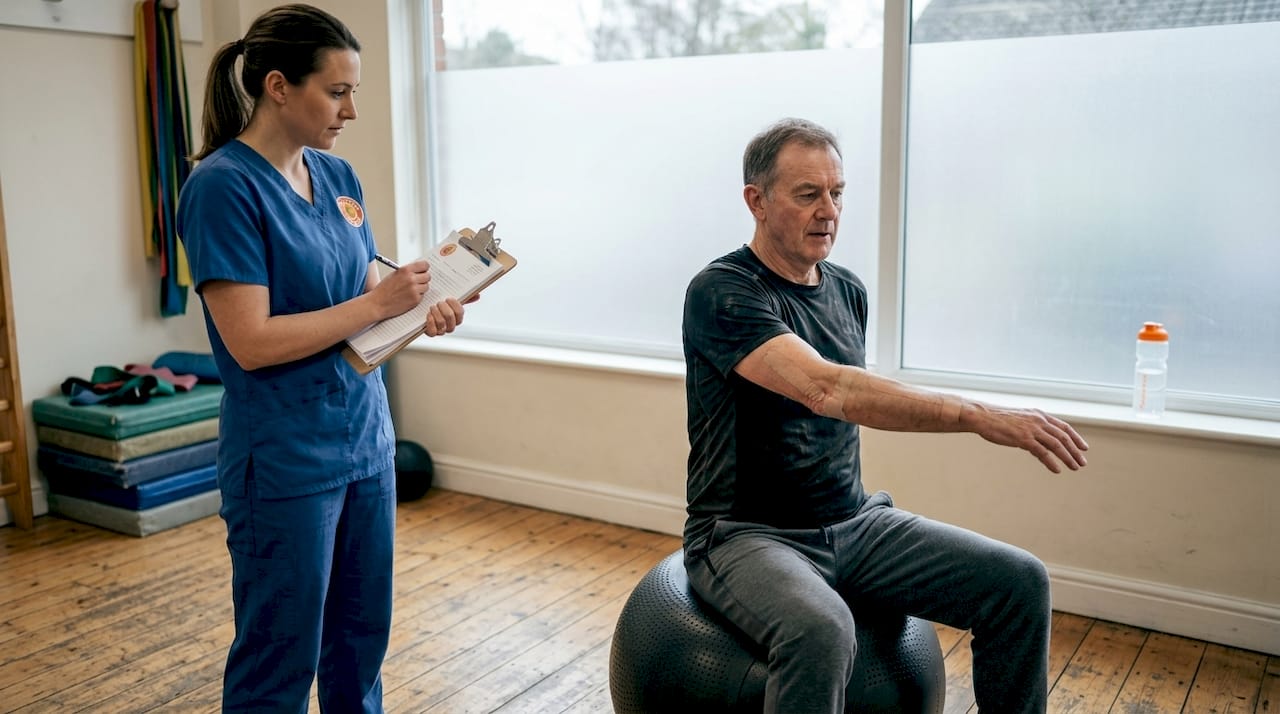
For sports injury patients, physiotherapy centres on targeted rehabilitation exercises that rebuild strength, restore movement patterns, and prevent re-injury. Your physiotherapist assesses biomechanical factors that may have contributed to the initial injury, then designs a progressive loading programme that safely returns you to sport. This approach recognises that tissue healing follows predictable timelines, but functional recovery requires deliberate, structured rehabilitation.
Post-operative care involves progressive mobilisation and biomechanical assessments to ensure proper healing whilst preventing compensatory movement patterns. Early physiotherapy intervention after surgery reduces complications, shortens hospital stays, and improves long-term outcomes. Your treatment plan balances the need for tissue protection during initial healing phases with the benefits of controlled movement that promotes circulation and prevents stiffness.
Manual therapy techniques, when integrated appropriately, act on nervous system modulation to reduce pain and improve function. These hands-on approaches complement exercise programmes by addressing movement restrictions and providing immediate symptom relief that enables you to engage more fully with active rehabilitation. The combination creates a synergistic effect that neither approach achieves alone.
Each patient receives a personalised physiotherapy plan based on:
Condition type and severity assessed through clinical examination
Individual goals related to work, sport, or daily activities
Previous treatment responses and medical history
Current fitness level and movement capacity
Psychological factors including pain beliefs and recovery expectations
Discover how Pilates integrates into rehabilitation programmes to enhance core stability and movement control. For sports-specific concerns, learn strategies for managing sports injury patients effectively throughout recovery.
Pro Tip: Ask your physiotherapist to explain the rationale behind each exercise in your programme so you understand how it contributes to your specific goals, which significantly improves adherence and outcomes.
Accessing physiotherapy for musculoskeletal disorders in Bedfordshire and Buckinghamshire
NHS musculoskeletal pathways in Bedfordshire and Buckinghamshire direct patients to appropriate diagnostic and treatment services quickly through structured triage systems. These pathways for back pain management ensure you receive timely assessment from qualified practitioners who determine whether physiotherapy, imaging, or specialist referral best suits your condition. The system aims to reduce waiting times whilst matching patients with the most appropriate level of care.
Private physiotherapy offers advanced modalities and flexible scheduling for adult patients who prefer immediate access or specialised treatments not routinely available through NHS services. Many private clinics provide extended appointment times that allow for comprehensive assessment and hands-on treatment during each session. This option suits patients with insurance coverage or those willing to invest in expedited care.
Access route | Assessment timeframe | Treatment options | Cost considerations |
NHS MSK pathway | 2-6 weeks typically | Standard physiotherapy, group classes | Free at point of use |
Private physiotherapy | Often within days | Extended sessions, advanced techniques | Self-pay or insurance |
Combined approach | Varies by pathway | Continuity between services | Mixed funding |
Early referral and active engagement in physiotherapy optimises long-term outcomes by preventing acute conditions from becoming chronic. When you address musculoskeletal problems promptly, you reduce the risk of compensatory movement patterns, muscle atrophy, and central sensitisation that complicate recovery. Waiting for symptoms to resolve spontaneously often extends overall recovery time and increases the likelihood of recurrence.
Collaborating with physiotherapists to customise treatment plans based on individual goals ensures your programme addresses what matters most to you. Whether you need to return to competitive sport, manage work-related demands, or simply walk without pain, your physiotherapist can prioritise interventions that target your specific functional requirements. This personalised approach improves motivation and adherence compared to generic exercise sheets.
Key factors when choosing your physiotherapy provider include:
Practitioner qualifications and specialisation areas relevant to your condition
Clinic location and appointment availability that fits your schedule
Treatment philosophy alignment with your preferences for active versus passive care
Insurance acceptance or transparent pricing for self-pay patients
Patient reviews and outcomes data demonstrating clinical effectiveness
Learn about creating personalised physiotherapy plans that align treatment with your unique recovery goals and lifestyle demands.
Pro Tip: Prepare for your first physiotherapy appointment by listing your main symptoms, activities that worsen or ease them, previous treatments tried, and your primary functional goals to maximise assessment efficiency.
Current research and future directions in physiotherapy for musculoskeletal disorders
Ongoing studies test optimal treatment frequency and duration for varied musculoskeletal disorder conditions to establish evidence-based protocols. Researchers examine whether intensive short-term interventions produce better outcomes than extended lower-frequency programmes, and how patient characteristics predict response to different dosing schedules. This work aims to personalise treatment intensity based on condition severity, chronicity, and individual recovery capacity.
Safety and cost-effectiveness are key evaluation metrics in new physiotherapy protocols as healthcare systems demand value-based care. Studies compare adverse event rates, quality-adjusted life years, and resource utilisation across different treatment approaches. High-quality randomised controlled trials are needed to determine optimal dosing, safety profiles, and multimodal physiotherapy effectiveness for specific musculoskeletal disorder populations.
Approach | Typical components | Potential benefits | Research gaps |
Unimodal physiotherapy | Single intervention focus | Clear outcome attribution | May miss synergistic effects |
Multimodal physiotherapy | Combined manual therapy, exercise, education | Addresses multiple pain mechanisms | Difficult to isolate active ingredients |
Stratified care | Treatment matched to risk profile | Efficient resource allocation | Requires validated screening tools |
Future research priorities to optimise physiotherapy outcomes include:
Identifying biomarkers that predict treatment response to enable precision medicine approaches
Evaluating digital physiotherapy delivery models for accessibility and effectiveness
Investigating optimal timing for physiotherapy intervention across different injury phases
Comparing supervised versus independent exercise programmes for long-term adherence
Examining psychological factors that mediate physiotherapy outcomes in chronic conditions
Testing implementation strategies that translate research findings into clinical practice
Emphasis on integration of manual therapies with exercise and education for best patient recovery reflects the understanding that no single intervention addresses all aspects of complex musculoskeletal disorders. Manual techniques may provide immediate symptom relief and improve movement quality, enabling more effective exercise participation. Education components enhance self-efficacy and reduce fear-avoidance behaviours that perpetuate disability. This tripartite approach targets biological, psychological, and social factors simultaneously.
Emerging technologies including wearable sensors, telerehabilitation platforms, and artificial intelligence-assisted assessment tools promise to enhance physiotherapy delivery and monitoring. These innovations may improve treatment precision, increase access for rural populations, and provide objective outcome data that informs clinical decision-making. However, research must establish whether technological enhancements translate to meaningful improvements in patient outcomes and satisfaction.
Explore various types of physiotherapy techniques to understand how different approaches may suit your specific condition and recovery goals.
Discover expert physiotherapy care tailored to your needs
Parks Therapy Centre offers personalised physiotherapy for chronic pain, sports injuries, and post-operative recovery throughout Bedfordshire and Buckinghamshire. Our experienced practitioners combine evidence-based manual therapy, progressive exercise prescription, and pain education to address your specific musculoskeletal disorder comprehensively.

Access specialist diagnostic imaging referrals and detailed biomechanical assessments on-site to ensure accurate diagnosis and targeted treatment planning. Early intervention with expert physiotherapy improves recovery speed and quality, reducing the risk of chronic symptoms that limit your daily function.
Book physiotherapy appointments online to streamline access to expert local care tailored to your recovery goals and lifestyle demands.
Frequently asked questions
What causes musculoskeletal disorders?
Musculoskeletal disorders arise from injury, degeneration, poor posture, and overuse that stresses tissues beyond their capacity. Acute injuries from sports or accidents cause immediate damage, whilst chronic conditions develop gradually through repetitive strain or age-related changes. Biomechanical factors including muscle imbalances, joint stiffness, and movement pattern dysfunction contribute to many musculoskeletal problems. Lifestyle factors such as sedentary behaviour, obesity, and occupational demands also increase risk for developing these conditions.
How long does physiotherapy take to improve musculoskeletal disorder symptoms?
Recovery time varies by condition severity, patient health, and adherence to therapy recommendations. Many patients notice improvement within two to four weeks of starting treatment, though full function restoration typically requires two to three months of consistent engagement. Chronic conditions that have persisted for years may need longer intervention periods to reverse established movement patterns and central sensitisation. Your physiotherapist will provide realistic timeframes based on your specific diagnosis and individual factors that influence healing.
What types of physiotherapy techniques are most effective for chronic musculoskeletal pain?
Exercise-based functional restoration with pain neuroscience education is the most effective approach for chronic musculoskeletal pain management. This combination addresses both physical deconditioning and unhelpful pain beliefs that perpetuate disability. Manual therapies targeting nervous system modulation complement exercise plans by providing immediate symptom relief and improving movement quality. Techniques including joint mobilisation, soft tissue work, and neural tension releases work through neurophysiological mechanisms rather than simply correcting structural problems.
How can I access physiotherapy services quickly in Bedfordshire or Buckinghamshire?
Use NHS musculoskeletal pathways for assessment and referral through your GP or by self-referring in areas where this option is available. These pathways typically provide initial assessment within two to six weeks depending on demand and urgency. Consider private physiotherapy for faster appointment availability and personalised care, often securing appointments within days of contact. Many private clinics accept insurance referrals or offer transparent self-pay pricing, making expert care accessible when you need prompt intervention to prevent acute problems becoming chronic.
Recommended
