How physiotherapy relieves pain: proven methods and benefits
- 5 hours ago
- 8 min read
TL;DR:
Physiotherapy offers non-invasive, personalized treatment that targets the root causes of pain.
Exercise, manual therapy, and education are evidence-based methods that improve long-term outcomes.
Active self-management through physiotherapy reduces medication dependence and enhances quality of life.
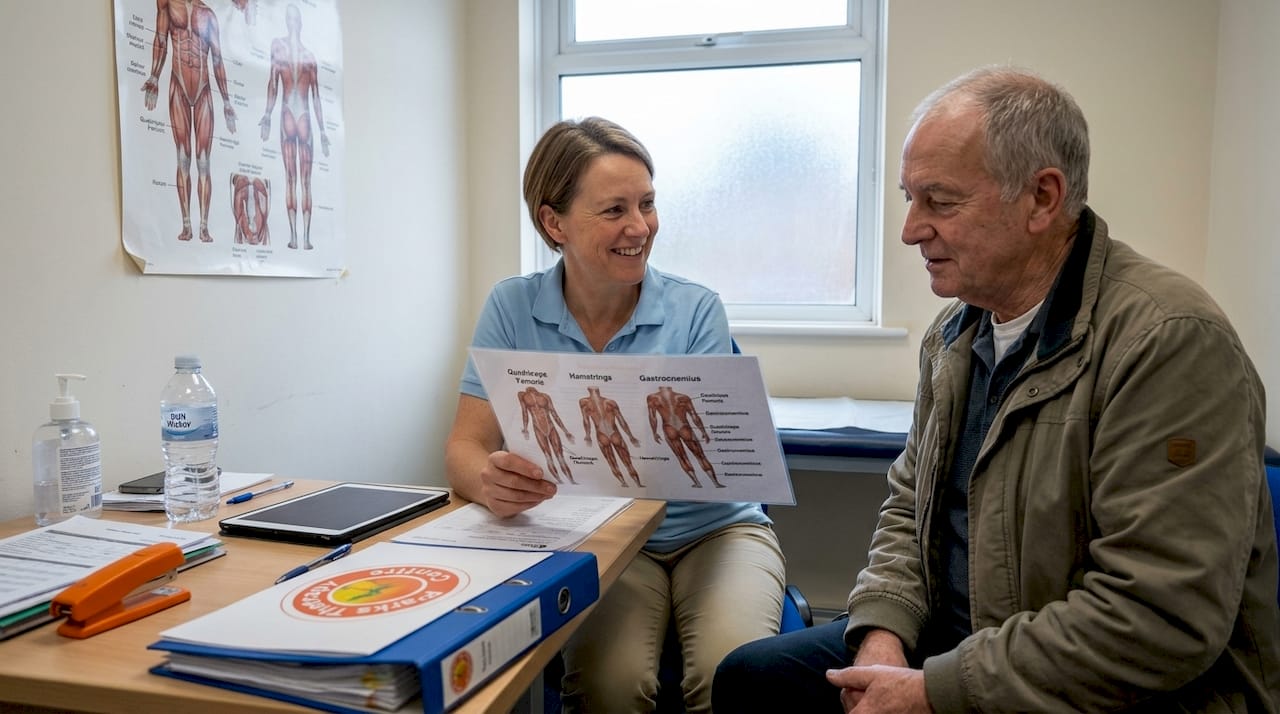
When pain takes hold, the instinct is often to reach for medication or assume surgery is the only answer. Yet physiotherapy uses non-invasive techniques that address the root cause of pain rather than masking it. For adults across Bedfordshire and Buckinghamshire living with chronic pain or musculoskeletal problems, this distinction matters enormously. In this article, you will learn how physiotherapy works, which methods carry the strongest evidence, and what practical steps you can take to manage pain more effectively and sustainably.
Table of Contents
Key Takeaways
Point | Details |
Personalised care matters | Physiotherapy works best when tailored to each person’s pain, goals, and challenges. |
Active methods outperform passive | Exercise, education, and self-management consistently offer better results than rest or quick fixes. |
Evidence guides effective care | Current research recommends combining physical and psychological strategies for lasting pain relief. |
Empowerment is key | Learning about pain and building self-confidence leads to long-term benefits and reduced reliance on medication. |
Understanding pain and why physiotherapy matters
Pain is not simply a signal that something is broken. It is a complex experience shaped by physical, psychological, and social factors. Acute pain, such as a sprained ankle, typically resolves as tissue heals. Chronic pain, which persists beyond three months, is a different matter entirely. It can reshape how your nervous system processes signals, making everyday tasks feel overwhelming and affecting sleep, mood, and independence.
For residents in Bedfordshire and Buckinghamshire, musculoskeletal conditions such as back pain, osteoarthritis, and neck problems are among the most common reasons people seek help. The impact on daily life is significant: reduced mobility, time off work, and a growing reliance on painkillers that may offer short-term relief but rarely resolve the underlying issue.
This is precisely where physiotherapy stands apart. Physiotherapy plays a central role in managing chronic pain and musculoskeletal issues, offering a whole-person approach that looks beyond the immediate site of pain. Rather than chasing a quick fix, physiotherapists assess how you move, how you think about your pain, and what your goals are.
Key advantages of physiotherapy for pain management include:
Non-invasive treatment that avoids the risks associated with surgery or long-term medication
Personalised assessment that identifies the specific drivers of your pain
Education and empowerment so you understand your condition and can manage it confidently
Functional focus on restoring movement, strength, and quality of life
Evidence-based methods supported by clinical research and physical therapy for pain guidelines
Local services are increasingly moving away from passive, one-off interventions towards sustained, physiotherapy guidance that supports long-term recovery. This shift reflects a deeper understanding of what chronic pain actually requires.
Statistic: Musculoskeletal conditions affect around 20% of the UK population at any one time, making effective, accessible physiotherapy more important than ever.
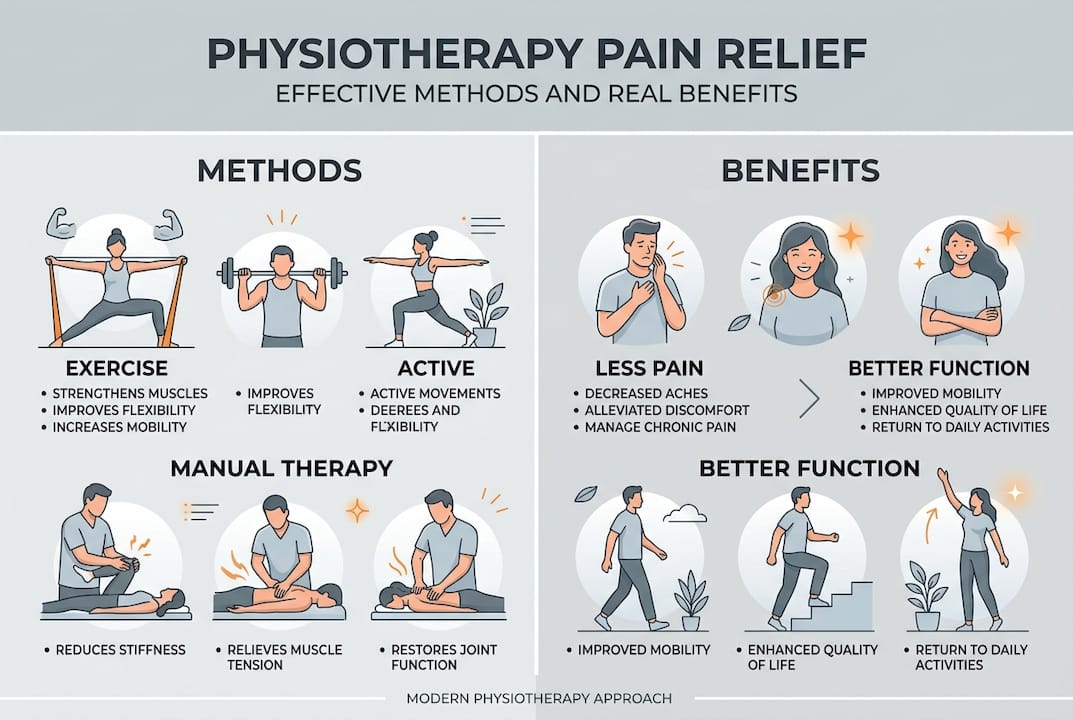
Core physiotherapy methods for pain management
With the foundation of why physiotherapy matters, let us break down the most effective methods physiotherapists use for pain management.
Exercise and manual therapy are highly effective for chronic pain, and most care pathways in Bedfordshire and Buckinghamshire will include a combination of the following:
Exercise therapy involves structured, progressive movement designed to build strength, flexibility, and endurance. It is the cornerstone of most physiotherapy programmes.
Manual therapy includes hands-on techniques such as joint mobilisation and soft tissue work to reduce stiffness and improve range of motion.
Pain neuroscience education (PNE) helps you understand why pain persists and how to break unhelpful cycles of avoidance.
Electrotherapy modalities such as TENS (transcutaneous electrical nerve stimulation) and therapeutic ultrasound may be used to complement the above.
Technique | Primary purpose | Evidence strength |
Exercise therapy | Strength, function, endurance | Strong |
Manual therapy | Mobility, pain reduction | Moderate to strong |
Pain education (PNE) | Fear reduction, self-efficacy | Moderate |
TENS/ultrasound | Symptom relief | Moderate |
Tailored exercise can yield up to 50% improvement in pain scores, which is a remarkable outcome for something that costs nothing beyond time and effort. The types of physiotherapy available are broader than most people realise, and a good physiotherapist will select and combine methods based on your specific presentation.

For physiotherapy home exercises, consistency between clinic sessions is what drives results. The chronic pain management literature consistently shows that patients who engage actively between appointments recover faster and maintain gains longer.
Pro Tip: Prioritise active treatments such as exercise over passive ones like heat packs or ultrasound alone. Passive treatments can provide temporary comfort, but active engagement is what builds lasting resilience.
Personalisation and psychological factors in physiotherapy
Having detailed the main methods, let us see why individualisation and understanding your mind’s role transforms results.
No two people experience pain in the same way, even when the diagnosis looks identical on paper. A 45-year-old office worker in Bedford with lower back pain will have entirely different needs from a retired teacher in Aylesbury with the same condition. Effective physiotherapy begins with a thorough assessment that covers not just physical function but also your goals, fears, and daily demands.
Psychological factors like catastrophising and movement fear significantly affect pain outcomes. Catastrophising, the tendency to expect the worst, can amplify pain signals and slow recovery. Fear of movement, known as kinesiophobia, leads people to avoid activity that would actually help them. A skilled physiotherapist recognises these patterns and addresses them directly through pain neuroscience education and graded exposure to movement.
Personalised care in physiotherapy typically involves:
Initial assessment covering movement, strength, pain behaviour, and lifestyle
Collaborative goal-setting so treatment aligns with what matters most to you
Regular monitoring to adjust the plan as you progress
Open communication about what is working and what needs to change
“The best physiotherapy is a conversation, not a prescription. When patients understand their pain and feel heard, they engage more fully and recover more completely.”
This is why starting physiotherapy with clear expectations and an open mind makes such a difference. Following a structured physiotherapy recovery steps plan that accounts for your psychological as well as physical state is far more effective than generic protocols.
Support from your physiotherapist between sessions, whether through written exercise plans, app-based tracking, or simple check-in calls, reinforces the sense that recovery is a shared endeavour rather than something done to you.
Nuances and what the latest evidence shows
Personalised care is powerful, but what does the latest research say about the best strategies for pain management?
Combining manual therapy and exercise leads to better short-term results than exercise alone for many musculoskeletal conditions. This does not mean manual therapy should replace exercise. Rather, the two work synergistically: hands-on treatment reduces pain and stiffness enough to allow more effective exercise, which then drives longer-term improvement.
Updated NICE recommends group exercise and cognitive therapies as first-line approaches for chronic primary pain, moving away from acupuncture and electrotherapies as standalone treatments. This is a significant shift that is already influencing how physiotherapy services in Bedfordshire and Buckinghamshire are structured.
Approach | Short-term benefit | Long-term benefit |
Exercise alone | Moderate | Strong |
Manual therapy alone | Moderate | Limited |
Combined approach | Strong | Strong |
Group exercise | Moderate | Moderate to strong |
It is worth noting that some comparisons in the research carry low certainty, meaning results vary between individuals and conditions. The physiotherapy vs chiropractic debate, for example, shows broadly similar outcomes for back pain, suggesting the quality of the therapeutic relationship and consistency of care matter as much as the specific technique.
Pro Tip: Ask your physiotherapist which specific evidence supports your treatment plan. A confident, qualified practitioner will welcome this question and use it to strengthen your understanding and commitment to recovery. Incorporating injury prevention with physio principles early also reduces the risk of setbacks.
Practical benefits: self-management and real-life outcomes
With an understanding of the evidence, let us focus on the real-world, practical difference physiotherapy can make in your daily life.
Physiotherapy empowers patients to reduce medication reliance and self-manage symptoms, and this is arguably its greatest long-term benefit. Moving away from a passive, medication-dependent approach towards active self-management is transformative for adults with chronic pain.
For most patients across Bedfordshire and Buckinghamshire, the practical outcomes of a well-delivered physiotherapy programme include:
Reduced pain intensity through targeted exercise and manual therapy
Improved mobility and strength that makes daily tasks easier and safer
Lower medication use as self-management skills replace the need for regular painkillers
Better sleep and mood as pain becomes less disruptive
Confidence to stay active without fear of causing further harm
Building these outcomes takes time, but the gains are durable. Unlike a course of medication that ends when the prescription runs out, the skills and habits developed through physiotherapy stay with you. Your physiotherapist will also guide you on arm rehabilitation or other specific recovery areas relevant to your condition.
Pro Tip: Keep a simple pain and activity diary during your treatment. Tracking small improvements, such as walking further or sleeping better, builds motivation and gives your physiotherapist the information needed to progress your plan effectively. Knowing how to prepare for physiotherapy sessions also helps you get more from every appointment.
Our perspective: what most pain management guides miss
Most pain management articles focus on techniques and evidence, which matters. But after years of working with patients in Bedfordshire and Buckinghamshire, we have seen something that rarely appears in clinical literature: the single biggest barrier to recovery is not the severity of pain. It is the belief that recovery is something that happens to you rather than something you actively build.
Patients who see their physiotherapist as a coach rather than a fixer consistently do better. They ask more questions, follow through on physio tips for beginners, and return to activity sooner. The relationship matters as much as the treatment itself.
Progress in pain management is rarely linear. There will be good weeks and difficult ones. What separates those who recover well from those who plateau is not talent or luck. It is the willingness to stay consistent through the difficult periods, guided by a physiotherapist who educates and empowers rather than simply applying hands-on treatment and sending you home.
Seek a practitioner who explains the why behind every exercise and decision. That transparency is not just good communication. It is good medicine.
Take your first step to pain relief with expert support
If you are ready to manage pain differently, and more effectively, the right support is closer than you think. At The Parks Therapy Centre, our experienced physiotherapists work across multiple locations in Bedfordshire and Buckinghamshire, delivering evidence-based, personalised care that goes far beyond short-term symptom relief.

Whether you are dealing with chronic back pain, a sports injury, or a long-standing musculoskeletal condition, we will carry out a thorough assessment and build a treatment plan around your goals. We also offer diagnostic imaging referrals where needed, ensuring nothing is missed. Book your assessment today and discover what physiotherapy in Bedfordshire and Buckinghamshire can genuinely do for your quality of life.
Frequently asked questions
How quickly can I expect pain relief from physiotherapy?
Exercise and manual therapy offer short-term pain relief for most people, and many notice meaningful improvement within 4 to 6 sessions, particularly when they commit to consistent home exercise between appointments.
Can physiotherapy help if medication hasn’t worked?
Yes. Physiotherapy aims for self-management and reduced medication reliance, and the evidence shows it can improve both pain levels and physical function even when medication alone has not delivered results.
What is pain neuroscience education (PNE)?
PNE enhances pain, function, and psychosocial results by teaching you how pain is processed in the body and brain, which reduces fear-driven avoidance and helps you return to movement with greater confidence.
Is group exercise better than one to one for chronic pain?
NICE recommends group exercise for many adults with chronic pain, but the ideal format depends on your specific condition, personal goals, and what you feel most comfortable with.
Recommended
