Effective physiotherapy for lateral epicondylitis: recover stronger
- Apr 11
- 7 min read

TL;DR:
Active physiotherapy, especially eccentric strengthening, is most effective for treating tennis elbow.
Progressive loading, manual therapy, and ergonomic modifications help ensure successful recovery and prevent recurrence.
Long-term management requires ongoing exercises, monitoring, and tailored plans, often over 12 to 18 months.
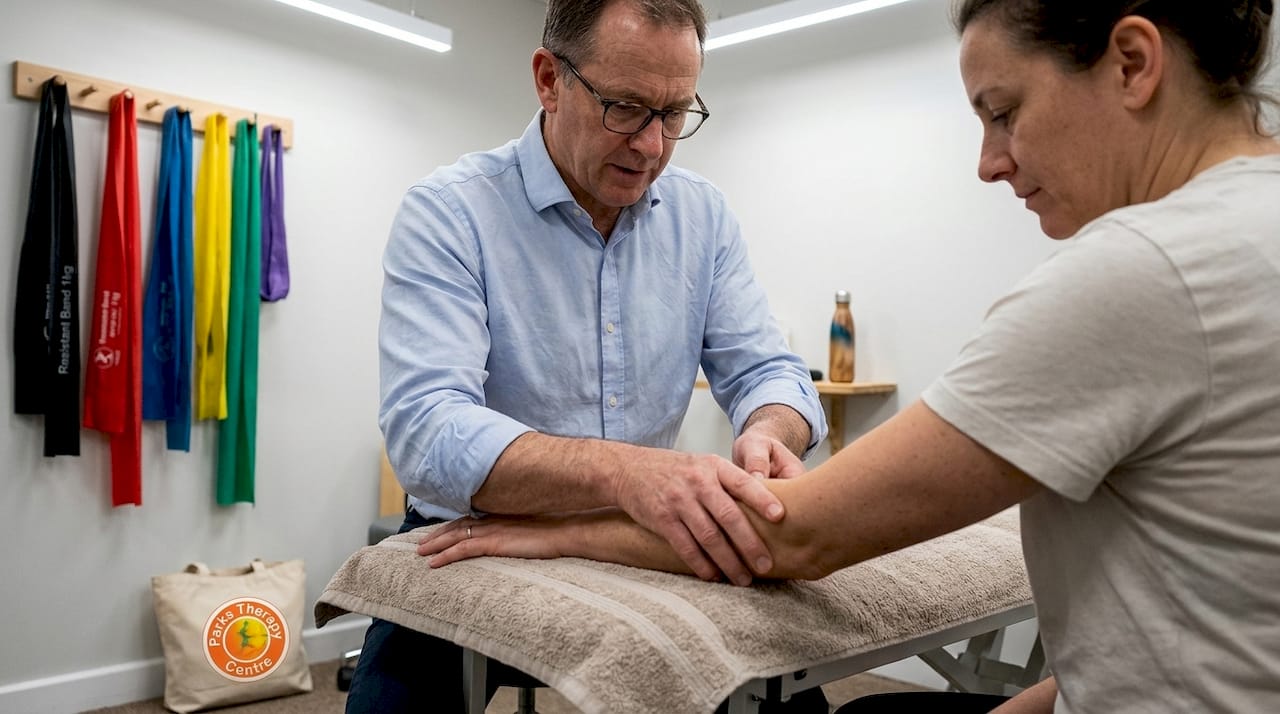
Rest alone will not fix tennis elbow. That belief has kept countless active adults on the sidelines far longer than necessary, watching their grip strength fade and their frustration grow. Lateral epicondylitis, the overuse injury affecting the outer elbow tendons, responds far better to active, structured physiotherapy than to passive waiting. Whether you are a weekend tennis player, a tradesperson doing repetitive arm work, or a gym regular, this guide will walk you through what the evidence actually says, which treatments work best, and how to build a recovery plan that fits your life.
Table of Contents
Key Takeaways
Point | Details |
Active rehab works best | Exercise and manual therapy are more effective than rest or passive treatments for lateral epicondylitis recovery. |
Eccentric exercises lead | Eccentric strengthening provides the greatest improvements in pain and function, especially with professional guidance. |
Personalise your plan | Recovery is most successful when physiotherapy is tailored to your activity level and daily demands. |
Monitor your progress | Regular assessment with grip strength and PRTEE helps track recovery and prevents recurrence. |
What is lateral epicondylitis and how does it affect you?
Lateral epicondylitis is an overuse injury of the tendons that attach to the lateral epicondyle, the bony prominence on the outer side of your elbow. Most people know it as tennis elbow, though the majority of sufferers have never held a racket. The condition develops when repetitive gripping, lifting, or twisting movements place more load on the forearm tendons than they can absorb, leading to micro-damage and a degenerative process within the tendon tissue itself.
The symptoms are usually hard to ignore:
A persistent ache or burning sensation on the outer elbow
Weakness when gripping objects such as a mug, tool, or steering wheel
Pain that worsens with wrist extension or forearm rotation
Tenderness directly over the lateral epicondyle
Discomfort that radiates down the forearm during daily tasks
It is not just athletes who are affected. Painters, plumbers, office workers, and musicians are all commonly diagnosed. The condition interferes with work, sport, and ordinary daily activities in ways that can feel disproportionate to the size of the injury.
“The good news is that 90% of cases resolve with conservative management within 12 to 18 months, particularly when progress is tracked using tools like the PRTEE questionnaire and pain-free grip strength tests.”
That recovery window is realistic, but it depends on the right approach from the start. Passive rest delays tendon adaptation. Active loading, guided by a physiotherapist, is what drives genuine healing. If you want to understand how to reduce your injury risk in the first place, our injury prevention guide covers the fundamentals well.
Core physiotherapy strategies: evidence-informed treatments
Once you understand the condition, the next question is simple: what actually works? The evidence points clearly towards active rehabilitation, with a few standout approaches.
Eccentric strengthening is the most well-supported intervention. Eccentric exercises involve the muscle lengthening under load, for example slowly lowering a weight with the wrist extended. Research shows eccentric exercises reduce pain by up to 42% on the Visual Analogue Scale and improve grip strength by up to 35%, with results even stronger when paired with manual therapy.
Treatment | Pain reduction | Grip strength gain | Best suited for |
Eccentric exercise alone | Up to 42% | Up to 35% | Most patients |
Manual therapy alone | Moderate short-term | Moderate | Early-stage or acute cases |
Eccentric + manual therapy | Greatest overall | Greatest overall | Most practical combination |
Heavy slow resistance (HSR) | Promising | Significant | Motivated, pain-tolerant patients |
Manual therapy, which includes joint mobilisation and soft tissue techniques, adds measurable benefit. Manual therapy versus sham reduces both pain and disability at the end of treatment, and multimodal approaches combining exercise with manual therapy consistently outperform no treatment for short-term outcomes.
Heavy slow resistance (HSR) training is generating interest as an emerging option. Pilot studies show significant PRTEE improvement with HSR protocols, but compliance is a real problem, with only 32% of participants completing the full programme due to pain aggravation. It is promising, but not yet a first-line recommendation for everyone.
Pro Tip: When choosing the right physiotherapy technique, always discuss your pain tolerance and daily schedule with your physiotherapist. A plan you can actually follow will always outperform a theoretically superior one you abandon after two weeks. Consistent home exercise tips can also bridge the gap between clinic sessions.
Tailoring physiotherapy to active lifestyles and athletes
For active adults and athletes, a generic protocol is rarely enough. Your physiotherapy plan needs to account for the demands of your sport or occupation, your current fitness level, and how quickly you need to return to full activity.
The key adaptations for active individuals include:
Shoulder and scapular stabilisation work: Weakness higher up the kinetic chain often contributes to overload at the elbow. Strengthening the rotator cuff and scapular stabilisers reduces the mechanical stress placed on the forearm tendons during throwing, racket sports, or overhead lifting.
Sport-specific loading progressions: Rather than generic wrist curls, your programme should gradually reintroduce the exact movement patterns your sport demands, starting at low intensity and building systematically.
Ergonomic modifications: Grip size on a racket, tool handle design, keyboard position, and lifting technique all influence how much load passes through the lateral elbow. Correcting these factors is as important as any exercise.
Technique review: Poor biomechanics are often a root cause. A physiotherapist can identify faulty movement patterns before they become reinjury triggers.
Canadian guidelines for epicondylitis specifically recommend including shoulder and scapular stabiliser work, sport-specific loading progressions, and ergonomic modifications for athletes and active individuals to prevent recurrence.
Pro Tip: Do not wait until you are pain-free to start thinking about return to sport. Reviewing our sports injury prevention strategies early in your rehab helps you plan a structured return rather than guessing when it is safe. If you are new to structured rehab, our beginner physiotherapy tips are a practical starting point.
Outcomes: measuring progress and preventing recurrence
Knowing your treatment plan is one thing. Knowing whether it is working is another. Measuring progress objectively keeps both you and your physiotherapist honest about what is and is not improving.
The three most reliable markers are:
PRTEE score: The Patient-Rated Tennis Elbow Evaluation is a validated questionnaire that scores pain and functional disability. Tracking this every two to four weeks reveals genuine trends rather than day-to-day fluctuations.
Pain-free grip strength: Measured with a dynamometer, this gives a concrete, reproducible number. Improvement here correlates strongly with return to function.
Pain-free range of movement: Wrist extension and forearm rotation should become progressively more comfortable as the tendon adapts.
“Conservative management over 12 to 18 months resolves 90% of lateral epicondylitis cases, with the PRTEE and pain-free grip strength serving as the most reliable outcome measures throughout recovery.”
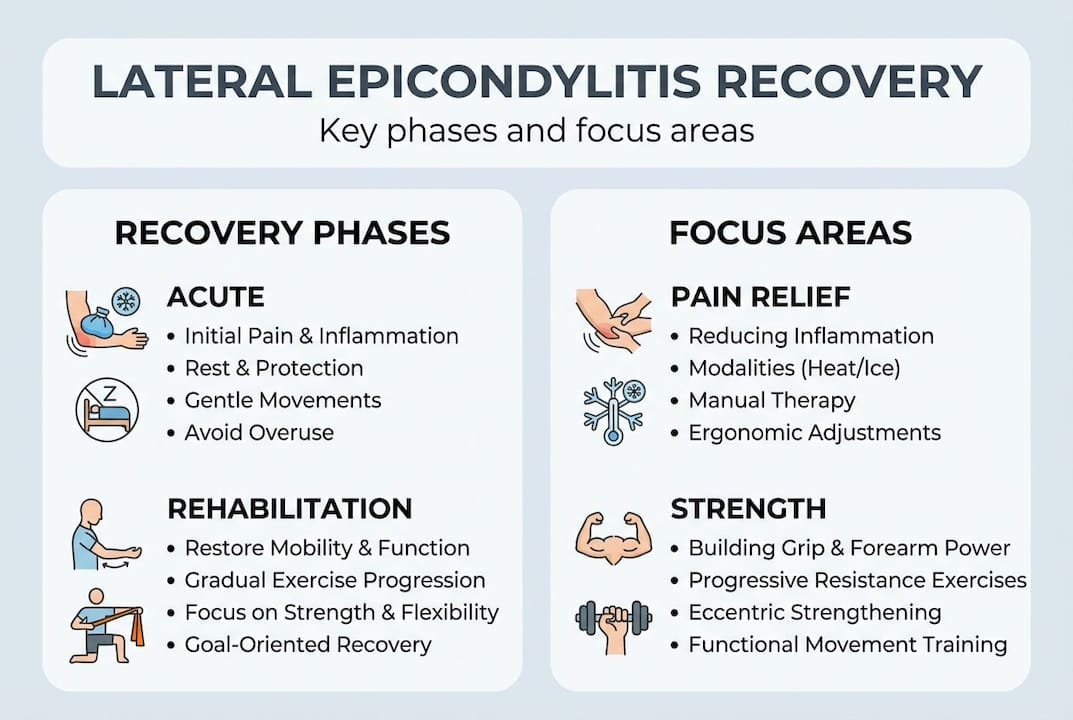
Recovery phase | Typical timeframe | Key focus |
Acute management | Weeks 1 to 4 | Pain reduction, gentle loading |
Progressive loading | Weeks 4 to 12 | Eccentric and isotonic strengthening |
Functional integration | Months 3 to 6 | Sport-specific or task-specific work |
Maintenance | Months 6 to 18 | Exercise continuation, ergonomic habits |
For long-term prevention, the evidence is clear: stopping your exercise programme the moment pain subsides is one of the most common reasons for recurrence. Continuing a maintenance programme, reviewing ergonomics periodically, and returning to activity gradually are the habits that keep lateral epicondylitis from coming back. Our injury assessment steps and guidance on managing injury recovery offer further detail on sustaining long-term results.
A physiotherapist’s perspective: what the evidence misses
The research on lateral epicondylitis is genuinely encouraging, but it can paint an overly tidy picture. Guidelines describe protocols. Real life is messier.
One thing the numbers rarely capture is how hard it is to stick with an intensive exercise programme when every repetition hurts. HSR training, for instance, shows impressive outcomes on paper, but a 32% completion rate tells you something important: pain is a powerful deterrent, and motivation alone is not enough to overcome it without ongoing clinical support.
Corticosteroid injections are another area where the evidence is often misread. They offer genuine short-term relief, which makes them attractive when pain is limiting daily function. But the longer-term data consistently shows that exercise-based recovery produces more durable results. The injection can feel like a solution when it is actually just a window of opportunity to begin proper loading.
What turns a protocol into a real outcome is the human element: incremental goal-setting, regular check-ins, and adjusting the plan when life gets in the way. If you are starting physiotherapy for the first time, knowing this upfront saves a lot of frustration.
Take your next step towards pain-free movement
Understanding the evidence is a strong foundation, but having expert support alongside you is what makes recovery consistent and sustainable.

At Parks Therapy Centre, our physiotherapists build bespoke rehabilitation programmes for lateral epicondylitis that account for your sport, your occupation, and your daily routine. We do not hand you a generic exercise sheet and send you home. We track your progress, adjust your plan as you improve, and help you stay on course when the process feels slow. If you are ready to move beyond guesswork and into guided recovery, book an assessment with our team and take the first concrete step towards lasting pain relief.
Frequently asked questions
How long does it take for lateral epicondylitis to heal with physiotherapy?
90% of cases resolve with conservative management within 12 to 18 months, and a physiotherapist can help you progress through recovery more efficiently by tailoring your programme from the outset.
What is the most effective exercise for lateral epicondylitis?
Eccentric strengthening exercises are most strongly supported by evidence, particularly when combined with manual therapy, as they reduce pain by up to 42% and improve grip strength significantly.
Can I keep training or playing sports with lateral epicondylitis?
Modified activity is usually possible, provided you follow a structured rehabilitation plan that includes sport-specific loading and ergonomic adjustments to avoid aggravating the tendon further.
Is heavy slow resistance (HSR) training better than traditional exercises?
HSR shows promise for faster gains, but low adherence due to pain means it is not suitable for everyone, and eccentric exercise remains the most consistently recommended approach.
Recommended
