Physiotherapy terminology explained: guide for patients
- Mar 22
- 10 min read
Walking into your first physiotherapy appointment, you’re met with a stream of unfamiliar terms: tendinopathy, eccentric loading, nociception. You nod along, but inside you’re lost. Understanding physiotherapy language isn’t just about sounding informed; it directly impacts how well you engage with treatment and recover. This guide demystifies the key musculoskeletal and sports injury terminology you’ll encounter in Bedfordshire and Buckinghamshire clinics, empowering you to participate actively in your care. Whether you’re managing a sports injury or supporting a loved one through rehabilitation, clear explanations will transform confusion into confidence.
Table of Contents
Understanding key physiotherapy terms for musculoskeletal and sports injuries
Core physiotherapy models and loading strategies in injury management
Advanced concepts and assessment tools in modern physiotherapy practice
Practical application: how understanding terminology improves your physiotherapy experience
Explore expert physiotherapy services in Bedfordshire and Buckinghamshire
Key Takeaways
Point | Details |
Strain vs sprain | Strains affect muscles or tendons and are graded from 1 to 3, while sprains involve ligaments and have a similar grade system but different healing timelines. |
Nociception versus pain | Nociception is the body’s detection system for potentially harmful stimuli, whereas pain is the brain’s conscious interpretation; you can have nociception without pain and pain without ongoing tissue damage. |
Tendinopathy types | Insertional tendinopathy affects where the tendon attaches to the heel bone and tends to present with morning stiffness, while midportion tendinopathy occurs 2 to 6 centimetres above the heel and worsens with running or jumping; treatment differs with insertional cases responding to lower load high repetition exercises and midportion benefiting from heavier eccentric loading. |
Positional versus postural | Clinicians distinguish positional from postural measurements, noting immediate spinal position versus habitual alignment to guide both short term positioning and long term behavioural changes. |
Symptom diary value | Keeping a symptom diary and using precise terminology when describing symptoms helps speed up accurate diagnosis and treatment planning. |
Understanding key physiotherapy terms for musculoskeletal and sports injuries
Physiotherapy consultations often involve technical language that can feel overwhelming. Let’s break down the fundamental terms you’ll encounter when dealing with common injuries in Bedfordshire and Buckinghamshire clinics.
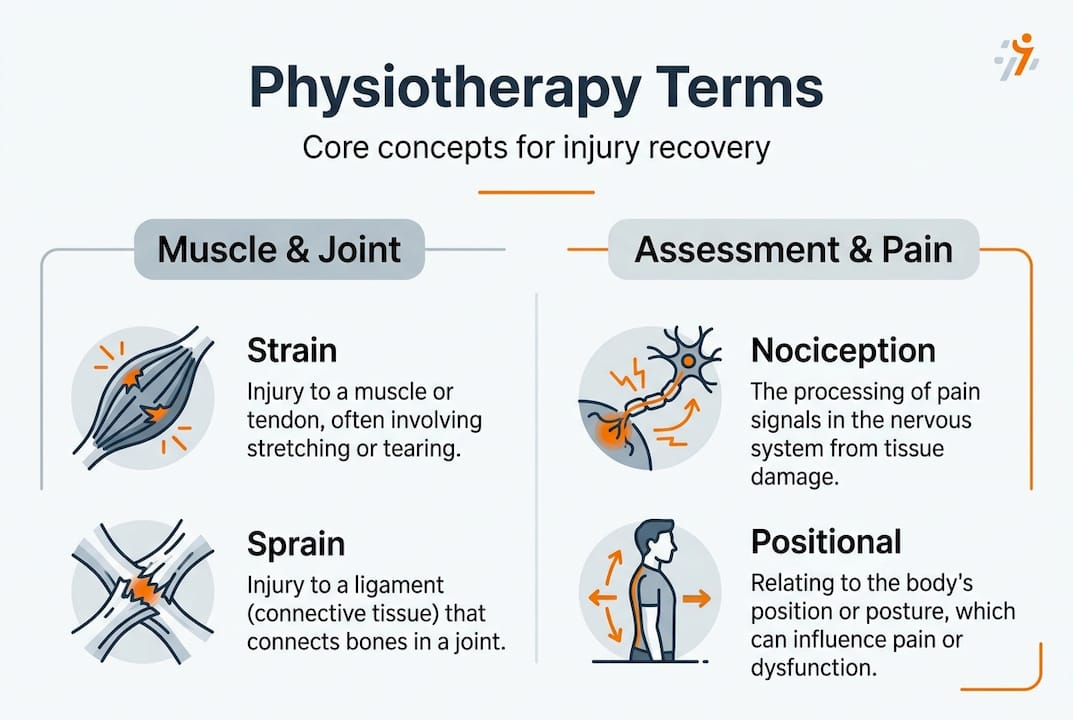
A strain affects muscles or tendons, the tissues connecting muscle to bone. When you overstretch or tear these structures, clinicians grade the injury from 1 to 3. Grade 1 involves mild overstretching with minimal fibre damage, Grade 2 indicates partial tearing with moderate pain and weakness, whilst Grade 3 represents complete rupture requiring potentially surgical intervention. A sprain, conversely, involves ligaments, the bands connecting bone to bone. The grading system mirrors strains, but the healing timeline and rehabilitation differ because ligaments have poorer blood supply.
Nociception describes your body’s detection system for potentially harmful stimuli. Specialised nerve endings called nociceptors send electrical signals to your spinal cord and brain when tissues experience mechanical stress, temperature extremes, or chemical irritation. This differs fundamentally from pain, which is your brain’s conscious interpretation of those signals. You can have nociception without pain (think of athletes who don’t notice injuries during competition) or pain without ongoing tissue damage (chronic pain conditions). This distinction matters because it helps you understand that persistent pain doesn’t necessarily mean your tissues are still injured, reducing anxiety and supporting recovery.
Achilles problems often involve two distinct conditions. Insertional tendinopathy affects where the tendon attaches to your heel bone, typically causing morning stiffness and pain when pushing off. Midportion tendinopathy occurs 2 to 6 centimetres above the heel, often presenting as a painful lump that worsens with running or jumping. The distinction matters because treatment protocols differ: insertional cases respond better to lower-load, higher-repetition exercises, whilst midportion injuries benefit from heavier eccentric loading.
In spinal assessments, clinicians distinguish between positional and postural measurements. Positional refers to where your spine sits at a specific moment, measured objectively with tools or visual assessment. Postural describes habitual alignment patterns over time, influenced by muscle strength, flexibility, and daily activities. Your physiotherapist might note that your spine is in 20 degrees of flexion positionally during an assessment, but your postural pattern shows excessive thoracic kyphosis from desk work. Understanding this helps you grasp why treatment addresses both immediate positioning and long-term habits. Following a step by step physiotherapy guide helps you track these changes systematically.
Pro tip: Keep a symptom diary noting when pain occurs, what activities trigger it, and its intensity. Use the correct terminology when describing symptoms to your physiotherapist, such as “sharp pain at the Achilles insertion when climbing stairs” rather than “my heel hurts sometimes.” This precision accelerates accurate diagnosis and treatment planning.
Core physiotherapy models and loading strategies in injury management
Modern physiotherapy relies on evidence-based frameworks that guide how clinicians progress your rehabilitation safely and effectively. Understanding these models empowers you to participate actively in treatment decisions.
The Load vs Capacity model explains injury mechanisms elegantly. Your tissues (tendons, muscles, bones) have a certain capacity to handle stress, determined by factors like strength, previous training, and recovery status. When the load you apply exceeds this capacity, whether through a single traumatic event or accumulated microtrauma, injury occurs. Rehabilitation aims to either reduce load temporarily (activity modification, technique correction) or increase capacity (strengthening exercises, gradual exposure). This framework helps you understand why rest alone rarely solves chronic problems; you must build capacity to handle the loads your lifestyle demands.
Progressive loading describes the systematic increase in exercise difficulty throughout rehabilitation. Your physiotherapist might start with isometric holds (muscle contraction without movement), advance to concentric exercises (muscle shortening under load), then introduce eccentric work (muscle lengthening under load), and finally add plyometric or sport-specific drills. Each stage builds capacity for the next. Regressive loading works in reverse, scaling back intensity when pain flares or capacity temporarily drops due to illness or overtraining. This bidirectional approach prevents the boom-bust cycle many patients experience.

Eccentric bias training has revolutionised tendinopathy management. During eccentric contractions, your muscle lengthens whilst producing force, like lowering a weight slowly or controlling your descent on a heel drop. Research demonstrates this loading pattern stimulates tendon remodelling more effectively than concentric or isometric work for conditions like Achilles tendinopathy. The gold standard protocol involves 3 sets of 15 repetitions twice daily for 12 weeks, with load progressed to maintain moderate discomfort (around 3-5 out of 10 on a pain scale) during the exercise.
Tendon stiffness refers to the tissue’s resistance to deformation under load. Contrary to popular belief, stiffer tendons aren’t necessarily problematic. In fact, optimal stiffness allows efficient force transmission from muscle to bone, improving athletic performance. However, tendons that are either too compliant (floppy) or excessively stiff relative to their strength can be injury-prone. Rehabilitation aims to optimise this property through progressive loading. Cumulative tendon load tracks the total stress your tendon experiences over days or weeks. A sudden spike, even if individual sessions seem manageable, often triggers symptoms. Monitoring cumulative load helps prevent overuse injuries.
Loading strategy | Primary indication | Key mechanism | Typical progression |
Isometric holds | Acute pain management | Pain inhibition without tissue strain | 5 x 45 seconds at 70% max effort |
Eccentric training | Chronic tendinopathy | Tendon remodelling and strength | 3 x 15 reps, increase load weekly |
Progressive loading | Post-injury rehabilitation | Gradual capacity building | Increase volume 10% weekly |
Plyometric training | Return to sport preparation | Power development and tissue resilience | Start at 50% max effort, progress to sport-specific drills |
Exploring various types of physiotherapy techniques helps you understand which loading strategies suit your specific condition and goals.
Pro tip: Progress your exercises based on how your symptoms respond 24 hours later, not just during the session. If pain increases significantly the next day or lasts beyond your warm-up, you’ve likely exceeded current capacity. Scale back 20-30% and rebuild gradually. Learning to manage sports injury patients effectively requires this responsive approach.
Advanced concepts and assessment tools in modern physiotherapy practice
Contemporary physiotherapy increasingly incorporates sophisticated assessment methods and technology to refine diagnosis and monitor rehabilitation progress objectively.
The distinction between insertional and midportion Achilles tendinopathy extends beyond anatomical location to therapeutic implications. Insertional cases often involve calcification within the tendon or at the bone interface, making them more complex and slower to resolve. These respond better to low-load, high-repetition protocols (LTCR: 4 sets of 30-40 repetitions at lighter resistance) that promote tendon adaptation without excessive compression at the bone attachment. Midportion tendinopathy typically presents with tendon thickening and responds optimally to high-load, low-repetition protocols (HTCR: 3-4 sets of 6-8 repetitions at 80-85% of maximum load). Research shows LTCR achieves superior outcomes for insertional pathology, whilst HTCR remains the evidence-based choice for midportion cases.
In spinal assessments, positional flexion measures your spine’s angle at a specific moment, often during movement analysis or postural screening. Your physiotherapist might note 45 degrees of lumbar flexion when you bend forward to touch your toes. Postural neutral, conversely, describes your spine’s habitual resting alignment, ideally maintaining natural curves (cervical lordosis, thoracic kyphosis, lumbar lordosis) without excessive deviation. Deviations from postural neutral, like increased thoracic kyphosis from prolonged sitting, create altered loading patterns that may contribute to pain over time. Treatment addresses both improving positional range and retraining postural habits.
Wearable technology has transformed injury monitoring and prevention. IMU-sEMG devices (inertial measurement units combined with surface electromyography) track both movement patterns and muscle activation simultaneously. Recent validation studies demonstrate these systems achieve 92.3% accuracy in classifying injury risk by analysing cumulative load, movement asymmetries, and fatigue patterns. For patients, this means objective data replacing subjective guesswork about when to progress activities or when you’re at heightened injury risk.
Assessment tool | What it measures | Clinical application | Accuracy |
IMU sensors | Movement patterns, joint angles, acceleration | Gait analysis, technique assessment, asymmetry detection | 95% for movement classification |
sEMG | Muscle activation timing and intensity | Fatigue monitoring, compensation patterns | 89% for activation pattern recognition |
Combined IMU-sEMG | Integrated movement and muscle data | Comprehensive injury risk profiling | 92.3% for injury-risk classification |
Force plates | Ground reaction forces | Loading asymmetry, power output | 98% for force measurement |
Clinicians use several key markers to personalise your treatment plan. These include pain response patterns (does it warm up or worsen with activity?), loading tolerance (how much weight or repetition before symptoms increase?), movement quality (compensatory patterns or asymmetries), and functional capacity (can you perform required daily or sport activities?). Tracking these markers over time reveals whether interventions are working and when to progress. Creating personalised physiotherapy plans depends on systematically monitoring these variables.
Technology enhances patient engagement by providing tangible evidence of progress. Seeing your movement symmetry improve from 65% to 88% over six weeks, or watching your cumulative load stay within optimal zones, reinforces adherence to rehabilitation protocols. This objective feedback often motivates patients more effectively than subjective reports alone. Understanding how to prepare for physiotherapy sessions includes familiarising yourself with these assessment tools.
Practical application: how understanding terminology improves your physiotherapy experience
Knowledge of physiotherapy terminology translates directly into better treatment outcomes and more satisfying healthcare experiences. Here’s how to leverage this understanding practically.
The NHS offers self-referral pathways for physiotherapy in many areas, including Bedfordshire and Buckinghamshire. You can access musculoskeletal services without seeing your GP first, reducing wait times. Typical treatments include exercise prescription tailored to your condition, manual therapy techniques like joint mobilisation or soft tissue work, education about pain mechanisms and self-management strategies, and advice on activity modification. Understanding these options helps you advocate for appropriate care and set realistic expectations.
Asking informed questions transforms passive appointments into collaborative problem-solving sessions. Instead of “Why does it still hurt?”, try “Given that I have midportion Achilles tendinopathy, should we consider increasing the load in my eccentric protocol, or does the persistent morning stiffness suggest I’m exceeding my current capacity?” This specificity helps your physiotherapist provide targeted advice efficiently. Similarly, describing symptoms using correct terminology (“I have sharp pain at the lateral epicondyle when gripping, especially after repetitive wrist extension”) enables faster, more accurate diagnosis than vague descriptions.
For carers supporting someone through rehabilitation, understanding clinical language helps you:
Reinforce exercise techniques correctly at home by knowing the difference between concentric and eccentric phases
Recognise warning signs that require clinical review, like distinguishing between expected post-exercise soreness and problematic pain increases
Communicate effectively with healthcare providers about observed changes in symptoms or function
Support appropriate activity pacing by understanding load management principles
Encourage adherence by explaining the evidence-based rationale behind prescribed exercises
Tracking symptoms and progress systematically improves outcomes. Document pain levels (0-10 scale) at consistent times, noting activities that increase or decrease symptoms. Record exercise compliance, including any modifications made due to pain. Note functional improvements, like stairs climbed without pain or distance walked comfortably. Take brief videos of exercise technique for your physiotherapist to review remotely if needed. This data helps clinicians adjust treatment precisely rather than relying on recall from weeks earlier.
Proactive collaboration yields the best results. Prepare questions before appointments. Share concerns about treatment progression honestly. Discuss barriers to exercise adherence (time constraints, gym access, confusion about technique) so your physiotherapist can problem-solve with you. Request clarification on any terminology you don’t understand; clinicians appreciate engaged patients who want to learn. Consider booking online at Parks Therapy Centre for convenient access to expert guidance, or explore bio-mechanical assessments for detailed movement analysis that informs personalised treatment.
Pro tip: Create a one-page summary of your condition using correct terminology, including your diagnosis, current treatment phase, exercise protocol, and progress markers. Share this with any healthcare provider you see (GP, specialist, different physiotherapist) to ensure continuity of care and consistent messaging. Update it monthly as your rehabilitation advances.
Explore expert physiotherapy services in Bedfordshire and Buckinghamshire
Now that you understand the language of physiotherapy, putting that knowledge into action with expert support accelerates your recovery. Parks Therapy Centre has served the Bedfordshire and Buckinghamshire communities since 1986, offering multidisciplinary care that demystifies complex terminology whilst delivering evidence-based treatment.

Our experienced physiotherapists specialise in translating clinical concepts into practical rehabilitation strategies tailored to your lifestyle and goals. Whether you’re managing a sports injury, recovering from surgery, or addressing chronic musculoskeletal pain, we’ll explain your diagnosis clearly and involve you actively in treatment decisions. Access diagnostic imaging referrals when needed for accurate diagnosis, or begin with comprehensive bio-mechanical assessments that identify movement patterns contributing to your symptoms. Ready to transform understanding into recovery? Book online at Parks Therapy Centre and experience the difference that clear communication and expert care make.
Frequently asked questions
What is the difference between a strain and a sprain?
A strain injures muscles or tendons (tissues connecting muscle to bone), whilst a sprain affects ligaments (tissues connecting bone to bone). Both use a Grade 1-3 classification system indicating severity, from mild overstretching to complete rupture. Strains typically heal faster due to better blood supply, but severe Grade 3 injuries of either type may require surgical repair.
How does understanding nociception help in managing pain?
Nociception describes your nervous system detecting potentially harmful stimuli, whilst pain is your brain’s interpretation of those signals. Recognising this distinction helps you understand that persistent pain doesn’t always indicate ongoing tissue damage, reducing anxiety and catastrophising. This knowledge supports engagement with active rehabilitation rather than excessive rest or avoidance behaviours that can perpetuate chronic pain.
Can I self-refer to physiotherapy in Bedfordshire or Buckinghamshire?
Yes, NHS self-referral pathways allow direct access to musculoskeletal physiotherapy services in many areas, including Bedfordshire and Buckinghamshire, without requiring a GP appointment first. This facilitates quicker assessment and treatment initiation. Contact your local NHS trust’s physiotherapy department or visit their website to complete a self-referral form, typically requiring basic information about your symptoms and medical history.
What are progressive loading exercises and why are they important?
Progressive loading involves systematically increasing exercise difficulty (weight, repetitions, speed, or complexity) throughout rehabilitation to build tissue capacity safely. This approach prevents both under-loading (insufficient stimulus for adaptation) and over-loading (exceeding current capacity and causing setbacks). It’s fundamental to modern rehabilitation because tissues adapt specifically to the demands placed on them, so graduated progression prepares you for the loads your lifestyle or sport requires whilst minimising re-injury risk.
Recommended
